Research on Open Innovation in Science
Our research team investigates the role and value of openness and collaboration in scientific research and science-based innovation. More specifically, we aim at exploring whether, and if so, how and under which conditions different forms and degrees of openness and inter/transdisciplinary collaboration influence the productivity and impact of scientific research.
Read more about our research on Open Innovation in Science here.
Seeing oneself as a data reuser: How subjectification activates the drivers of data reuse in science
The paper investigates which factors influence whether scientific researchers actually make use of the unprecedented volume of data being shared these days.
LaFlamme, M., Poetz, M., & Spichtinger, D., 2022. Seeing oneself as a data reuser: How subjectification activates the drivers of data reuse in science. PloS one, 17(8), e0272153.
Organizing for inter- and transdisciplinary collaboration in science: the role of autonomy vs. control
The paper sheds light on how organizational design choices – related to exercising control vs. granting autonomy – influence the scientists’ engagement in inter- and transdisciplinary research collaborations.
Beck, S., LaFlamme, M., Poetz, M.K. 2022. Organizing for inter- and transdisciplinary collaboration in science: the role of autonomy vs. control. Academy of Management Proceedings, 2022(1), 1698.
Crowdsourcing research questions in science
The paper shows that involving citizens more in the early stages of research studies could be key to generating new, innovative perspectives and promoting impactful research. More specifically, on average the crowdsourced questions are less novel and scientifically relevant, but the top 20% of research questions developed by citizens outperform those of experts on all dimensions.
Beck, S., Brasseur, T.M., Poetz, M. and Sauermann, H., 2022. Crowdsourcing research questions in science. Research Policy, 51(4), p.104491.
Special Issue on Open Innovation in Science
This special issue focuses on ‘Open Innovation in Science’ (OIS) as a novel concept that provides a unifying frame to study openness and collaboration in scientific research.
Special Issue on Open Innovation in Science (Eds: Susanne Beck, Christoph Grimpe, Marion Poetz and Henry Sauermann), 2022, published in Industry and Innovation, 29(2).
Crowds, citizens, and science: a multi-dimensional framework and agenda for future research.
This paper clarifies the relation between Crowd Science and Citizen Science, proposes a framework to profile CS projects, also accommodating machines and algorithms, and outlines a research agenda anchored on important underlying organizational challenges of CS projects.
Franzoni, C., Poetz, M., & Sauermann, H. 2022. Crowds, citizens, and science: a multi-dimensional framework and agenda for future research. Industry and Innovation, 29(2), 251-284
The Open Innovation in Science Research Field: A Collaborative Conceptualisation Approach.
In this paper, 47 authors collaboratively link dispersed knowledge on Open Innovation, Open Science, and related concepts such as Responsible Research and Innovation by proposing a unifying Open Innovation in Science (OIS) Research Framework. The paper highlights both tensions and commonalities between existing approaches.
Beck, S., Bergenholtz, C., Bogers, M., Brasseur, T.-M., Conradsen, M. L., Di Marco, D., Distel, A. P. Dobusch, L., Dörler, D., Effert, A., Fecher, B., Filiou, D., Frederiksen, L., Gillier, T., Grimpe, C., Gruber, M., Haeussler, C., Heigl, F., Hoisl, K., Hyslop, K., Kokshagina, O., LaFlamme, M., Lawson, C., Lifshitz-Assaf, H., Lukas, W., Nordberg, M., Norn, M. T., Poetz, M. K., Ponti, M., Pruschak, G., Pujol Priego, L., Radziwon, A., Rafner, J., Romanova, G., Ruser, A., Sauermann, H., Shah, S. K., Sherson, J. F., Suess-Reyes, J., Tucci, C. L., Tuertscher, P., Vedel, J. B., Velden,T., Verganti, R., Wareham, J., Wiggins, A., and Xu, S. M. 2022. The Open Innovation in Science Research Field: A Collaborative Conceptualisation Approach. Industry and Innovation , 29(2), 136-185.
Experimenting with Open Innovation in Science (OIS) practices: A novel approach to co-developing research proposals.
This paper summarizes and reflects on both the process and outcome of a novel experiment to co-develop scientific research proposals in the field of Open Innovation in Science (OIS), wherein scholars engaged in the study of open and collaborative practices collaborated with the “users” of their research, i.e., scientists who apply such practices in their own research. The resulting co-developed research proposals focus on scientific collaboration, open data, and knowledge sharing and are available as an appendix.
Beck, S., Bercovitz, J., Bergenholtz, C., Brasseur, T. M., D’Este, P., Dorn, A., Doser, M., Dosi, C., Effert, A., Furtuna, R., Goodyear, M., Grimpe, C., Hans, F., Haeussler, C., Heinisch, B., Katona, N., Kleinberger-Pierer, H., Kokshagina, O., LaFlamme, M., Lawson, L., Lehner, P., Lifshitz-Assaf, H., Lukas, W., Marchini, S., Mitterhauser, M., Moscato, F., Nordberg, M., Norn, M. T., Poetz, M., Ponti, M., Pruschak, G., Rafner, J. F., Romasanta, A. K., Ruser, A., Sameed, M., Sauermann, H., Suess-Reyes, J., Tucci, C. L., Tuertscher, P., Vicente Sáez, R., Vignoli, M., and Zyontz, S. 2021. Experimenting with Open Innovation in Science (OIS) practices: A novel approach to co-developing research proposals. CERN IdeaSquare Journal of Experimental Innovation, 5(2), 28-49.
Examining Open Innovation in Science (OIS): What Open Innovation can and cannot offer the science of science.
This paper seeks to clarify and refine the meaning and ambition of OIS and gives real-world examples of how OIS approaches in Denmark and the Netherlands are helping to rebalance priorities and lay the groundwork for future breakthroughs.
Beck, S., LaFlamme, M., Bergenholtz, C., Bogers, M., Brasseur, T.-M., Conradsen, M. L., Crowston, K., Di Marco, D., Effert, A., Filiou, D., Frederiksen, L., Gillier, T., Gruber, M., Haeussler, C., Hoisl, K., Kokshagina, O., Norn, M. T., Poetz, M. K., Pruschak, G., Pujol Priego, L., Radziwon, A., Ruser, A., Sauermann, H., Shah, S. K., Suess-Reyes, J., Tucci, C. L., Tuertscher, P., Vedel, J. B., Verganti, R., Wareham, J., Xu, S. M. 2021. Examining Open Innovation in Science (OIS): What Open Innovation can and cannot offer the science of science. Innovation (2021): 1-15.
Measuring the innovation impact of scientific research: exploring the potentials of artificial intelligence.
In this paper, we explore the potential of machine learning to assess how scientific publications inform practice guidelines and as such shape actual decision-making in society.
Distel, A., Grimpe, C., Körner, S., Landhäusser, M., and Poetz, M.K. 2021. Measuring the innovation impact of scientific research: exploring the potentials of artificial intelligence. Academy of Management Best Paper Proceedings.
The value of scientific knowledge dissemination for scientists – A value capture perspective
By taking a value capture perspective, this article conceptualizes and explores how individual scientists capture value from disseminating their knowledge.
Beck, S., Mahdad, M., Beukel K., Poetz, M. 2019. The value of scientific knowledge dissemination for scientists – A value capture perspective. Publications, 7(3), 1-23.
Impact
What is Societal Research Impact? A literature review.
Here you find a short Literature Review on Societal Research Impact and how it is evaluated and developed in different countries.
Impact of RTI policies on the relation between science and society
A reflection on the role of Austrian Research Technology and Innovation (RTI) policies aiming at participatory approaches in research in improving the relationship between science and society. The document enables a shared understanding of the assessment of the impact of such policies, proposes concrete measures to deepen the understanding of the role that RTI policies can play in improving the relationship between science and society in the Austrian context.
More reports: On the impact of RTI policies on social innovation and on a green economy
Co-Developing an impact model for evaluating the societal impact of participatory research approaches
This paper sets out to describe the co-creative development of an Impact Model and Reflection Instruments by different stakeholders that make desired and expected societal effects of participatory research visible, and enable a systematic evaluation of these expected changes.
Priority Setting
Involving Stakeholders in Research Priority Setting
In our scoping review „Involving Stakeholders in Research Priority Setting“ we present how stakeholders have thus far been involved in priority setting. The review describes, synthesizes, and evaluates research priority setting projects not only for the field of health – as previous reviews have done – but does so on a much broader scale for any research area. By mapping out the complex landscape of stakeholder involvement in research priority setting, this review guides future efforts to involve stakeholders effectively, inclusively, and transparently, which in turn may increase the overall value of research for society.
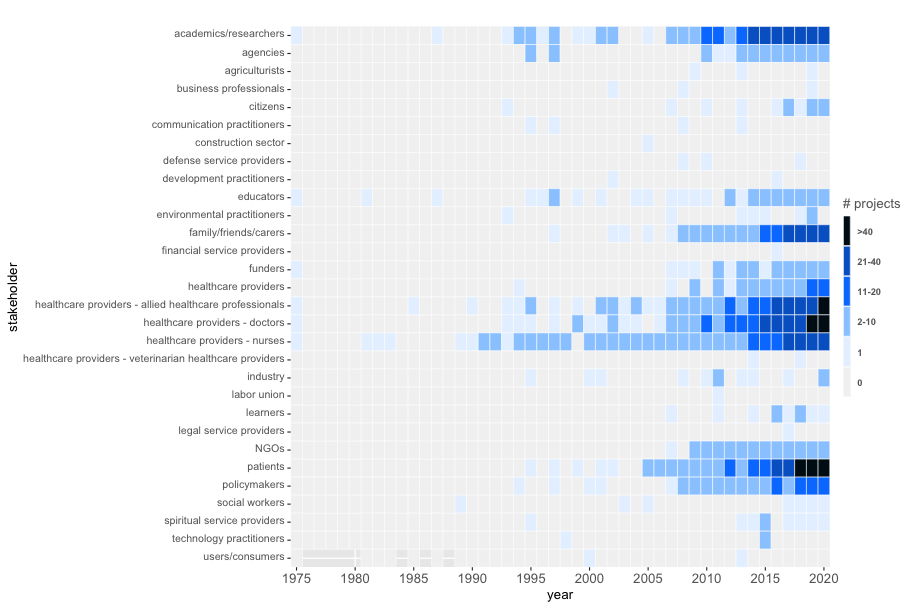
Patient and public involvement (PPIE) in (health) research
How do stakeholders view their participation in transdisciplinary research?
Working collaboratively and openly together with stakeholders has become a common phenomenon in research, however the stakeholder perspective on this is yet unknown. This paper reveals the enablers and barriers for such collaborations from the viewpoint of stakeholders and how they perceive such collaboration.
Kaisler, R.E. and Grill, C., 2021. Enabling Transdisciplinary Collaboration: Stakeholder Views on Working With “Children With Mentally Ill Parents” Research Groups. Frontiers in psychiatry, 12.
Introducing patient and public involvement practices to healthcare research in Austria: strategies to promote change at multiple levels.
Patient and public involvement (PPI) in research is well-established in the UK, but it can be challenging to introduce PPI to research communities where there is limited prior knowledge, experience or appreciation of PPI. This paper explores current PPI practices, experiences and ethical and operational challenges with PPI within our own research community in Austria, to inform strategies for supporting PPI in Austria going forward.
Kaisler, R. E., Kulnik, S. T., Klager, E., Kletecka-Pulker, M., Schaden, E., & Stainer-Hochgatterer, A., 2021. Introducing patient and public involvement practices to healthcare research in Austria: strategies to promote change at multiple levels. BMJ open , 11(8), e045618.
Co-creating a patient and public involvement and engagement ‘how to’ guide for researchers.
In this project, the authors invited a multi-stakeholder group consisting of researchers from multiple disciplines, citizen scientists, youth and patient advocates to co-create a guide on ‘how to’ meaningfully involve citizens in research.
Kaisler, R. E., & Missbach, B., 2020. Co-creating a patient and public involvement and engagement ‘how to’guide for researchers. Research involvement and engagement, 6(1), 1-10.
Evidence-based Practice and Polices for Impact on Mental Health of Children and Adolescents
Novel forms of engagement increase the opportunity to generate innovative problem-solving approaches. In this case study, the “Village project”, the authors investigate different measures aiming to drive evidence-based change, towards making a sustainable impact for children that have a parent with a mental illness.
Kaisler, R. E., & Paul, J. L., 2019. Evidence-based practice and polices for impact on mental health of children and adolescents. fteval Journal for Research and Technology Policy Evaluation, (48), 114-119.
PPIE literature Databases from external sources
Patient-Centered Outcomes Research Institute (PCORI) Literature Database
NIHR INVOLVE evidence library
NIHR INVOLVE Case Studies
Further PPIE literature from external sources
In this classic paper, Arnstein describes the different levels of participation in science and society. In this work, Arnstein makes an attempt to discuss the typology of citizen participation from her experiences with federal social programs, including urban renewal, anti-poverty, and Model Cities. Based on this, Arnstein developed levels of citizen participation arranged as rungs on a ladder, with each rung corresponding to the amount of “citizen control” within the process of determining a program or policy.
Arnstein, S. R. 1969. A ladder of citizen participation. Journal of the American Institute of Planners, 35(4), 216-224.
Meaningful patient engagement (PE) can enhance the development of medicines. However, the current PE landscape is fragmented and lacks comprehensive guidance. The authors systematically searched for PE initiatives. Multistakeholder groups integrated these with their own PE expertise to co-create a draft of PE Quality Guidance which was evaluated by public consultation. Projects exemplifying good PE practice were identified and assessed against the PE Quality Criteria to create a Book of Good Practices. Seventy-six participants from 51 organizations participated in nine multistakeholder meetings (2016–2018). The cocreated INVOLVE guidelines provided the main framework for PE Quality Guidance and were enriched with the analysis of the PE initiatives and the PE expertise of stakeholders. Seven key PE Quality Criteria were identified. The PE Quality Guidance was generally agreed to be useful for achieving quality PE in practice, understandable, easy to use, and comprehensive.
Deane, K., Delbecque, L., Gorbenko, O., Hamoir, A. M., Hoos, A., Nafria, B., … & Brooke, N. (2019). Co-creation of patient engagement quality guidance for medicines development: an international multistakeholder initiative. Bmj Innovations, bmjinnov-2018.
There are numerous frameworks for supporting, evaluating and reporting patient and public involvement in research. The literature is diverse and theoretically heterogeneous. This article aims to identify and synthesize published frameworks, consider whether and how these have been used, and apply design principles to improve usability. The plethora of frameworks combined with evidence of limited transferability suggests that a single, off-the-shelf framework may be less useful than a menu of evidence-based resources which stakeholders can use to co-design their own frameworks.
Greenhalgh, T., Hinton, L., Finlay, T., Macfarlane, A., Fahy, N., Clyde, B., & Chant, A. 2019. Frameworks for supporting patient and public involvement in research: Systematic review and co‐design pilot. Health Expectations.
In this rapid review, a systematic approach to research papers covering co-design processes along the research cycle is depicted. Results show that research co-design appears to be widely used but seldom described or evaluated in detail. Though it has rarely been tested empirically or experimentally, existing research suggests that it can benefit researchers, practitioners, research processes and research outcomes. Realizing the potential of research co-design may require the development of clearer and more consistent terminology, better reporting of the activities involved, and better evaluation.
Slattery, P., Saeri, A. K., & Bragge, P. 2019. Research co-design in health: a rapid review. Open Science Framework.
In recent years, there has been considerable interest in finding out what difference patient and public involvement makes in research projects. Researchers gain an understanding of involvement through their direct experience of working with patients and the public. This is ‘knowledge in context’ or ‘insight’ gained in the same way that patients gain expertise through their direct experience of a health condition. This means that detailed accounts of involvement from researchers already provide valuable learning to others, in the same way that patients’ insights help shape research. However, the impact of involvement will always be somewhat unpredictable, because at the start of any project, researchers ‘don’t know what they don’t know’—they do not know precisely what problems they might anticipate until the patients/members of the public tell them.
Staley, K. 2015. ‘Is it worth doing?’ Measuring the impact of patient and public involvement in research. Research involvement and engagement, 1(1), 6.
